Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
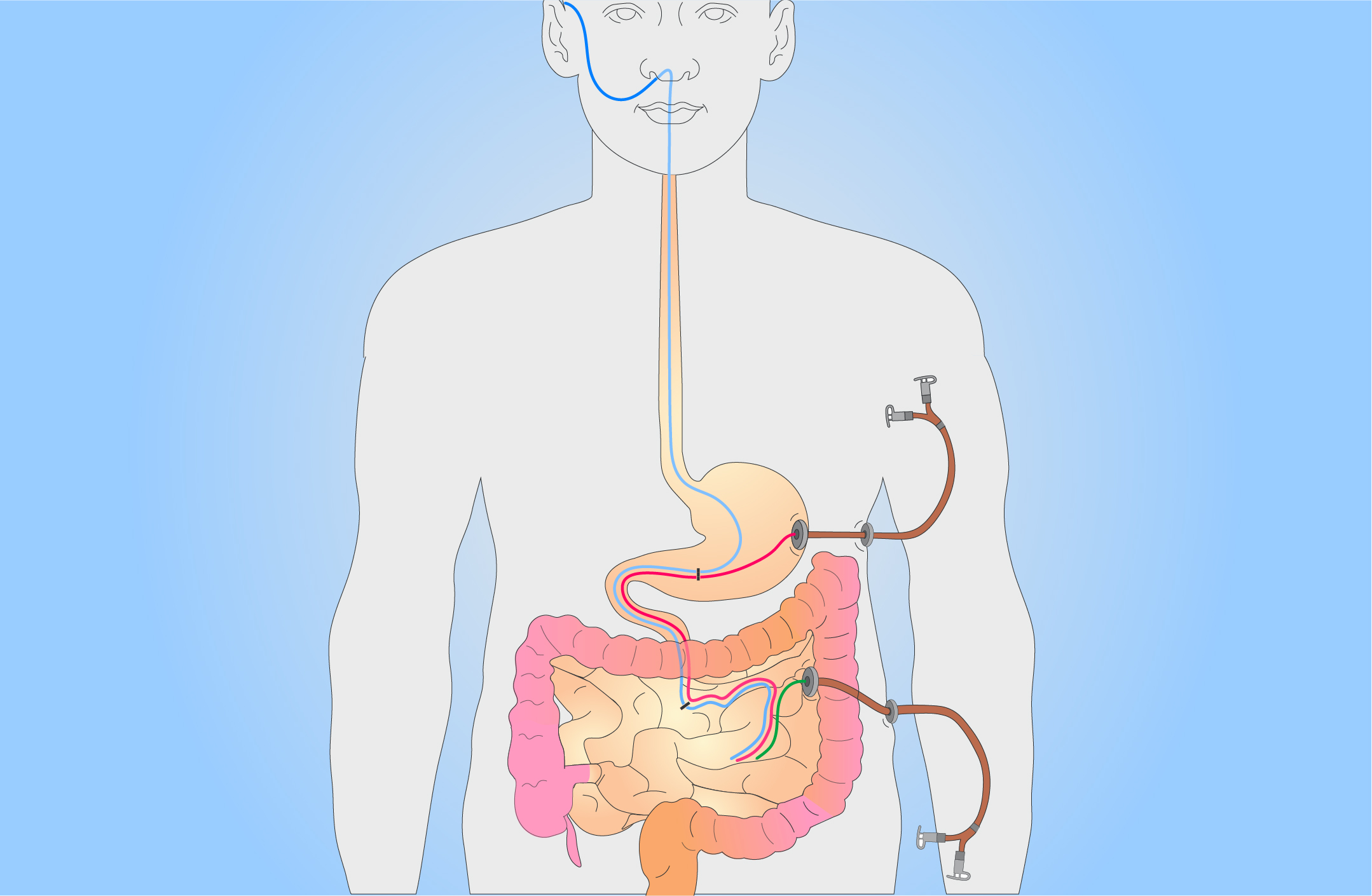
Enteral nutrition
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
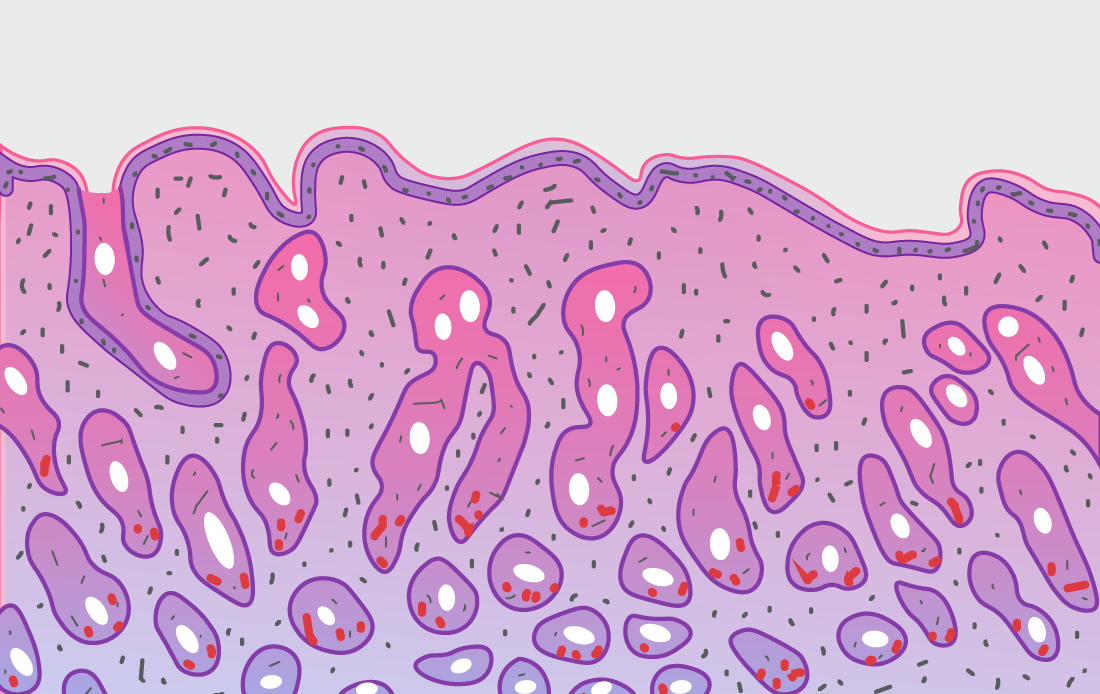
The diagnosis and management of coeliac disease and gluten-related disorders
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
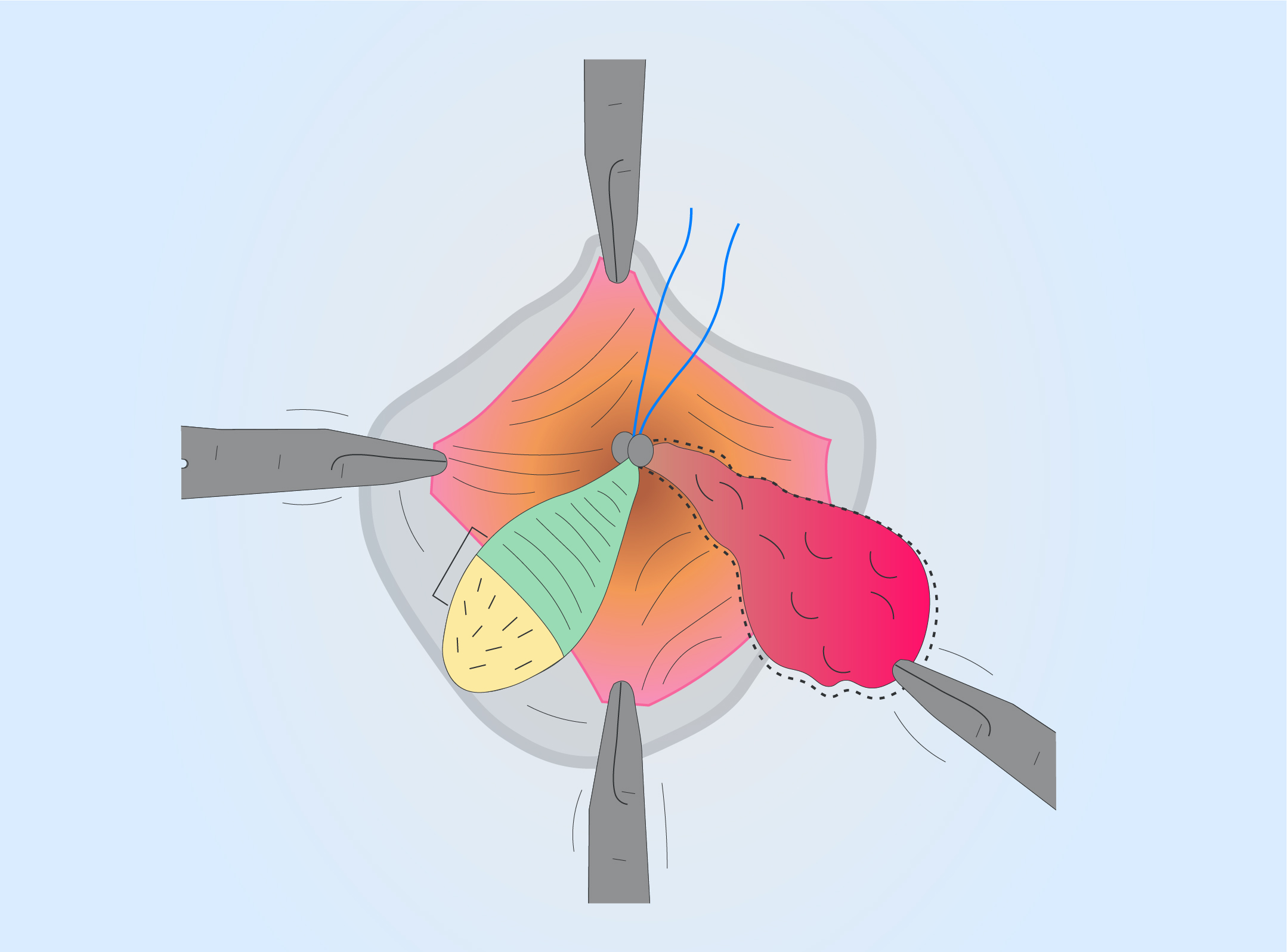
Proctology — haemorrhoids and perianal skin conditions
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
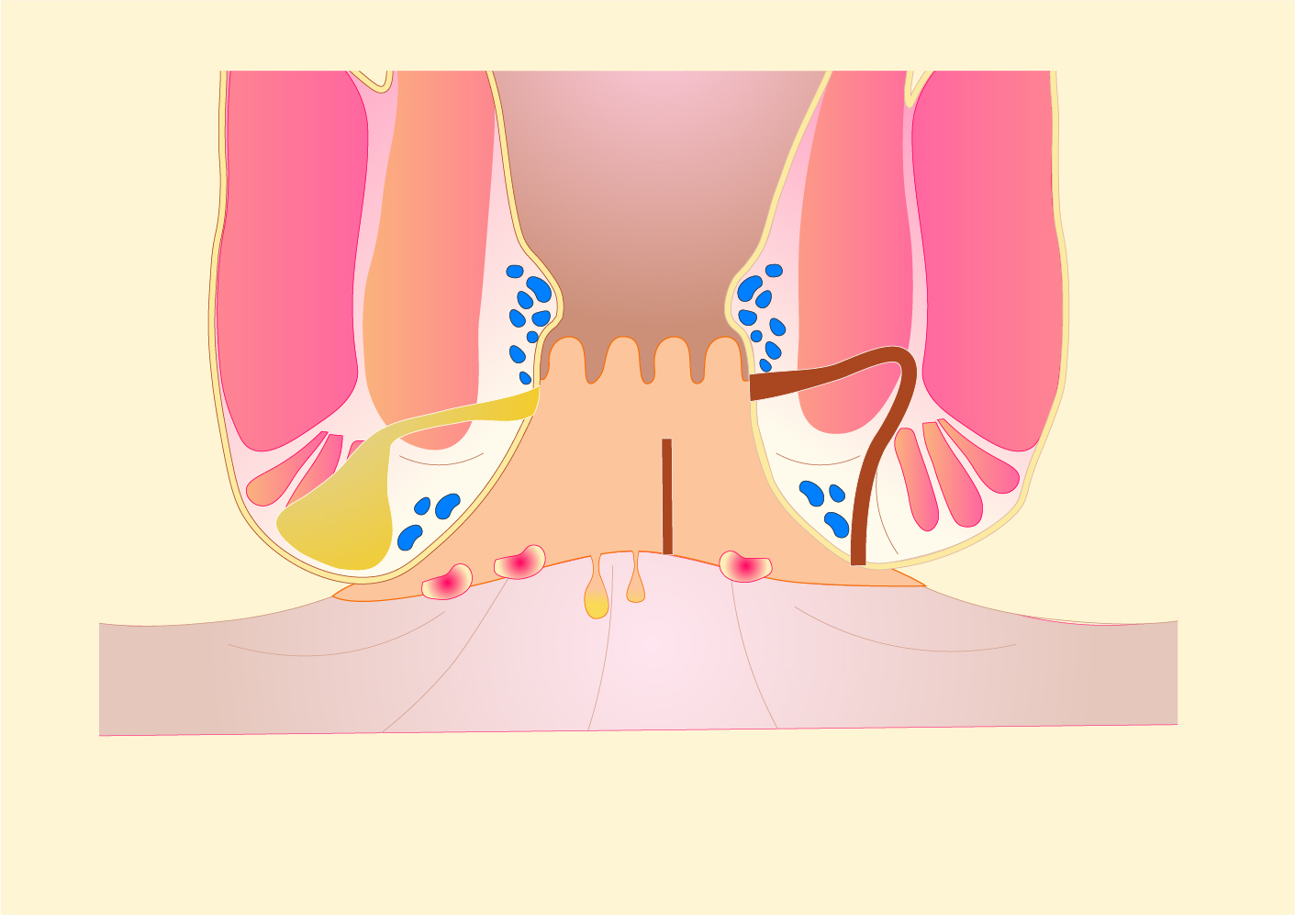
Perianal Crohn's disease
Event
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
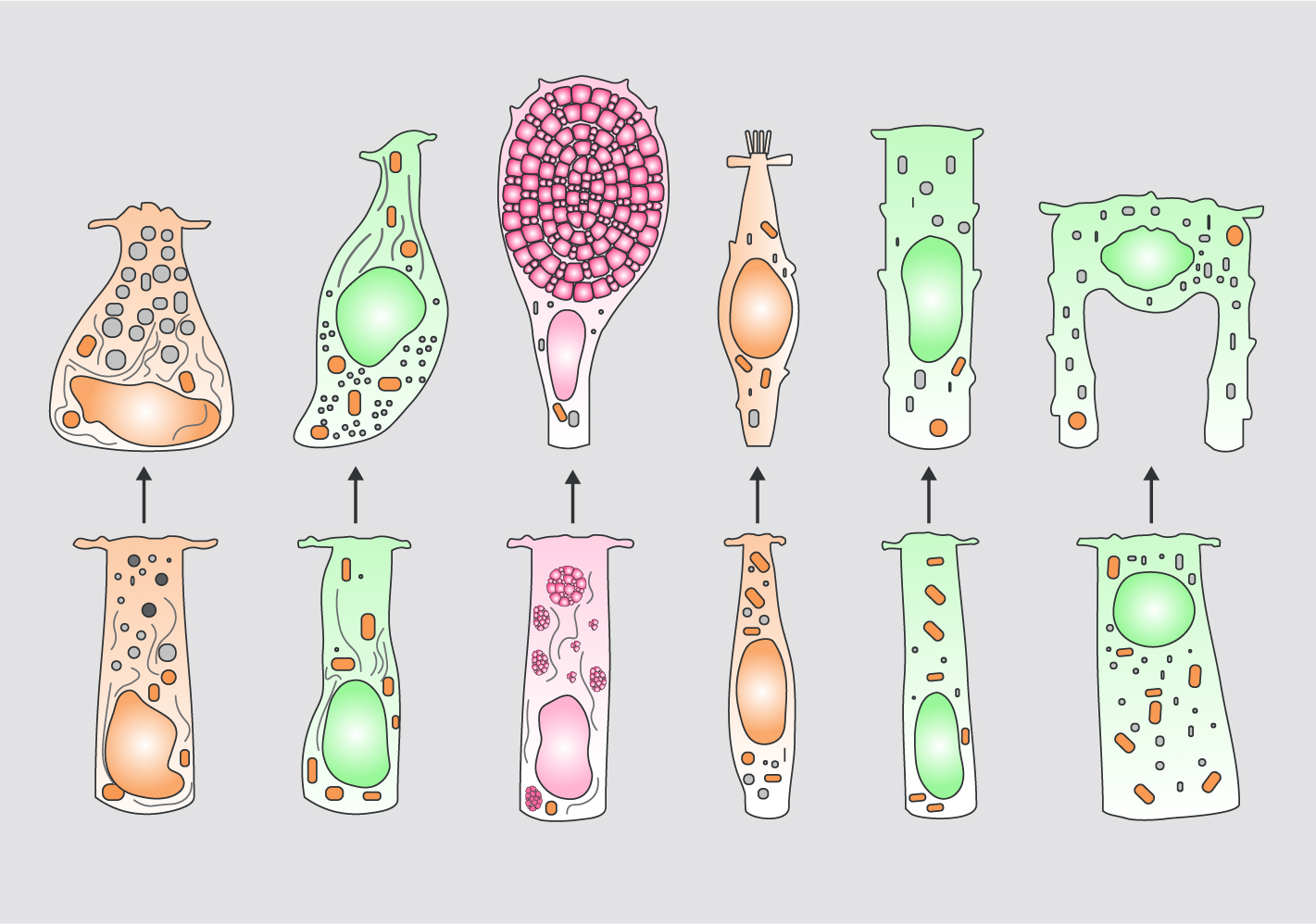
Gastroenterologist's guide to stem cells
Event
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

TREATMENT PATTERNS AND DISEASE PROGRESSION AMONG PATIENTS WITH EOSINOPHILIC OESOPHAGITIS IN EUROPE: A REAL-WORLD STUDY
Ulrike von Arnim 1, Frank Zerbib 2, Tiffany Pela 3, Amr Radwan 4, Juby Jacob-Nara 3, Bram P. Raphael 4, Rohan C. Parikh 5, Fareedat Bello 5, Gaelle Le-Bagousse-Bego 6, Ryan Thomas 4, Sarette Tilton 3
1 University Hospital, Magdeburg, Germany
2 CHU de Bordeaux, Centre Médico-Chirurgical Magellan, Hôpital Haut-Levêque, Department of Gastroenterology, Université de Bordeaux, INSERM CIC 1401, Bordeaux, France
3 Sanofi, Cambridge, MA, United States
4 Regeneron Pharmaceuticals, Inc., Sleepy Hollow, NY, United States
5 RTI Health Solutions, Research Triangle Park, NC, United States
6 Sanofi, Chilly-Mazarin, France
Conference
Topics
Submission format
Citation
Published

Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
Laudatio UEG Lifetime Achievement Awardee
1 Leiden University Medical Center, Leiden, Netherlands
Event
Session