Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
Infectious Colitis
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
Proctology — haemorrhoids and perianal skin conditions
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
Intestinal failure and parenteral nutrition
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
Gastroenterologist's guide to stem cells
Event
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
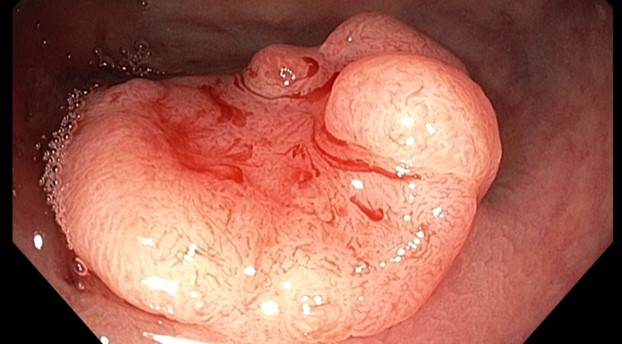
Management of early-invasive (T1) colorectal cancer
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

SERUM VILLIN-1 LEVEL – A TELL-TALE SIGN OF GUT BARRIER FAILURE IN CIRRHOTIC PATIENTS WITH ACUTE DECOMPENSATION
David Tornai 1, Boglarka Balogh 1, Aniko Csillag 1, Andras Budai 2, Andras Kiss 2, Tamas Dinya 1, Gabor Mehes 1, Lukacs Barath 1, István Tornai 1, Zsuzsanna Vitális 1, Nora Sipeki 1, Tamás Tornai 3, Peter Antal-Szalmas 1, Jonel Trebicka 4, Mária Papp 1
1 University of Debrecen, Faculty of Medicine, Debrecen, Hungary
2 Semmelweis University, Faculty of Medicine, Budapest, Hungary
3 Semmelweis University, Budapest, Hungary
4 University of Münster, Münster, Germany|||European Foundation for Study of Chronic Liver Failure, Barcelona, Spain
Conference
Topics
Submission format
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

PREDICTORS OF EOSINIPHILIC ESOPHAGITIS IN PATIENTS WITH DYSPHAGIA AND NORMAL ENDOSCOPY
Filippo Ovidi 1, Pierfrancesco Visaggi 1, Irene Solinas 1, Emanuele Marciano 2, Jason M. Dunn 3, Terence Wong 3, Edoardo Vincenzo Savarino 4, Nicola de Bortoli 1, Sebastian S. Zeki 3
1 Gastroenterology Unit, University of Pisa, Pisa, Italy
2 Azienda Ospedaliero Universitaria Pisana, Pisa, Italy
3 St Thomas' Hospital, London, United Kingdom
4 University of Padua, Division of Gastroenterology, Padua, Italy
Conference
Topics