Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
A primer in capsule endoscopy
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
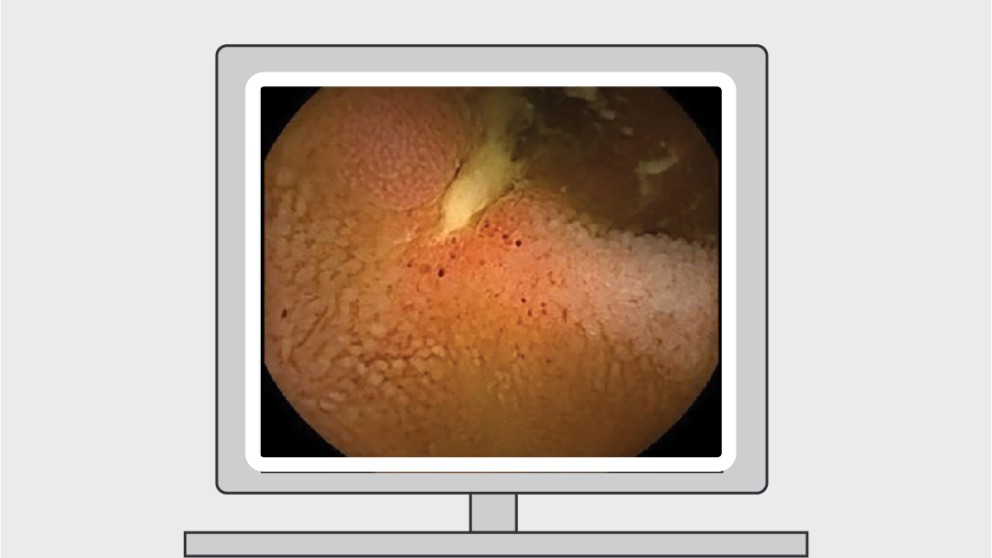
Mistakes in capsule endoscopy and how to avoid them
Topics
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

IMPACT OF NEW TIMING RECOMMENDATIONS FOR CAPSULE ENTEROSCOPY IN THE SETTING OF OVERT DIGESTIVE BLEEDING
Maria Manuela Estevinho 1, Rolando Pinho 1, Adélia Rodrigues 1, Unknown Unknown 1, Joao Paulo Laranjeira Correia 1, Pedro Silva Mesquita 1, Teresa Freitas 1
1 Centro Hospitalar Vila Nova de Gaia Espinho, Vila Nova de Gaia, Porto, Portugal
Conference
Topics
Submission format
Session
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

CIRCULATING BLOOD MICROBIOME SIGNATURES OF HEPATOCELLULAR CARCINOMA ARE ASSOCIATED WITH TREATMENT RESPONSE AND PROGNOSIS
Rolandas Gedgaudas 1, Egidijus Morkunas 1, Ruta Inciuraite 2, Alexander Link 3, Jurgita Skieceviciene 2, Marianna Alunni-Fabbroni 4, Kerstin Schütte 5, Peter Malfertheiner 4, Greta Varkalaite 2, Jens Ricke 4, Juozas Kupcinskas 1
1 Lithuanian University Of Health Sciences, Kaunas, Lithuania|||Lithuanian University Of Health Sciences, Kaunas, Lithuania
2 Lithuanian University Of Health Sciences, Kaunas, Lithuania
3 Otto-von-Guericke University of Magdeburg, Magdeburg, Germany
4 Univeristy Hospital of LMU Munich, Munich, Germany
5 Marienhospital Osnabrück, Osnabrück, Germany|||Medizinische Hochschule Hannover, Hannover, Germany
Conference
Topics
Submission format
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

A NOT SO COMMON MEDICAL COMPLICATION OF ENDOSCOPIC PROCEDURE
1 Mansoura Specialized Medical Hospital, Mansoura, Egypt
Conference
Topics
Submission format
Session
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

UTILIZATION OF HANDCRAFTED SOFTWARE FOR QUANTITATIVE CONTRAST-ENHANCED HARMONIC EUS-FOCUSING ON DIFFERENTIAL DIAGNOSIS OF PANCREATIC TUMORS
1 Far Eastern Memorial Hospital, New Taipei City, Taiwan, Province of China|||Graduate Institute of Biomedical Electronics and Bioinformatics, National Taiwan University, Taipei, Taiwan, Province of China|||Taiwan Contrast EUS Study Group, Taipei, Taiwan, P
2 Graduate Institute of Biomedical Electronics and Bioinformatics, National Taiwan University, Taipei, Taiwan, Province of China
3 Taiwan Contrast EUS Study Group, Taipei, Taiwan, Province of China|||National Taiwan University Hospital, Taipei, Taiwan, Province of China|||National Taiwan University, Taipei, Taiwan, Province of China
4 Taiwan Contrast EUS Study Group, Taipei, Taiwan, Province of China|||National Taiwan University, Taipei, Taiwan, Province of China|||National Taiwan University Hospital, Taipei, Taiwan, Province of China
Conference
Topics
Submission format
Session
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

RELATIVE ASSOCIATION OF BOWEL URGENCY CLINICALLY MEANINGFUL IMPROVEMENT AND BOWEL URGENCY REMISSION VS STOOL FREQUENCY REMISSION AND RECTAL BLEEDING REMISSION WITH IMPROVEMENT IN WPAI SCORES IN PATIENTS WITH MODERATELY TO SEVERELY ACTIVE ULCERATIVE COLITI
Bruce E. Sands 1, Brian G. Feagan 2, Theresa Hunter Gibble 3, Anthony Keohane 3, William J. Eastman 3, Kristina Traxler 3, Stefan Schreiber 4, Vipul Jairath 5, Alessandro Armuzzi 6
1 Icahn School of Medicine at Mount Sinai, New York, United States
2 The University of Western Ontario, London, Canada
3 Eli Lilly and Company, Indianapolis, United States
4 University Hospital Schleswig-Holstein, Kiel, Germany
5 Western University, London, Canada
6 IBD Center, IRCCS Humanitas Research Hospital, Rozzano, Milan, Italy
Conference
Topics
Submission format
Session