Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
Mistakes in dietary management of IBS and how to avoid them
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
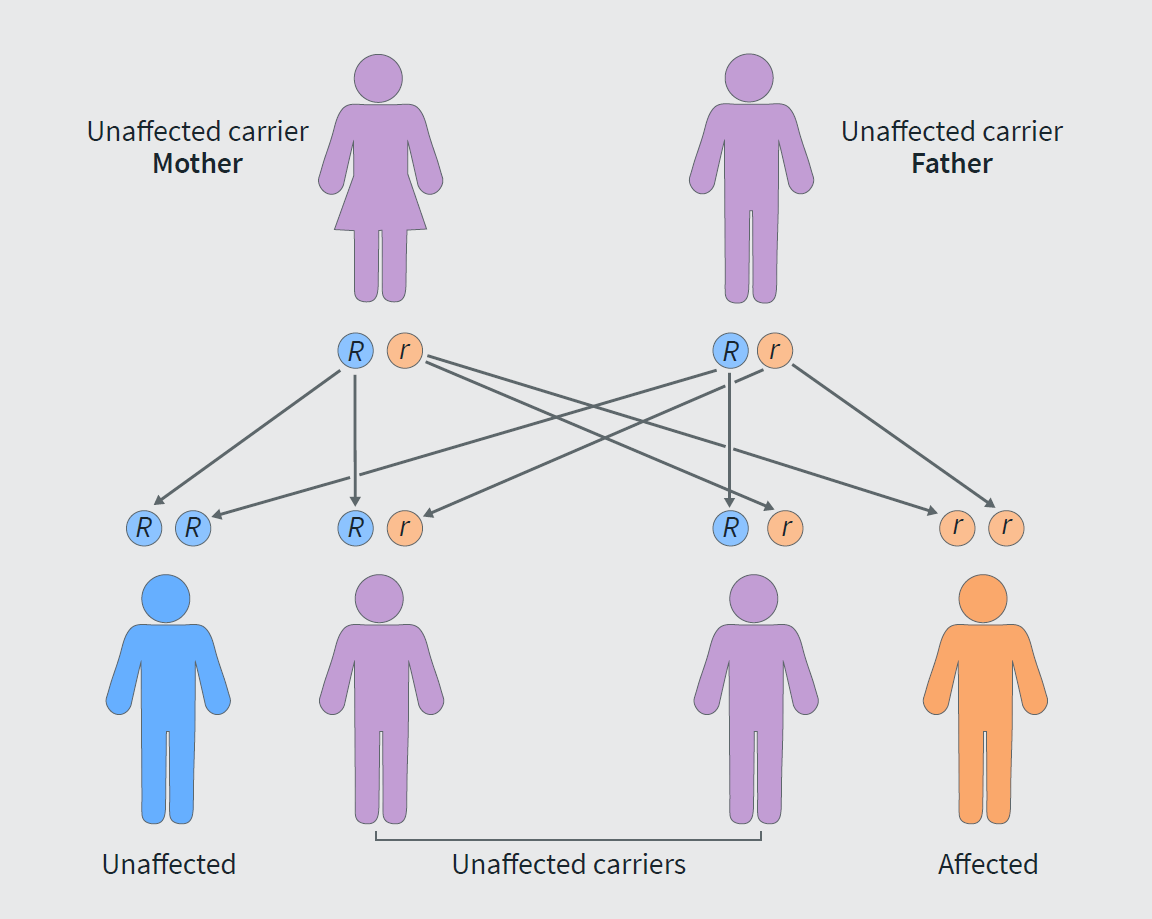
Mistakes in Familial Mediterranean Fever and how to avoid them
Topics
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

Mistakes in the management of carbohydrate intolerance and how to avoid them
Topics
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
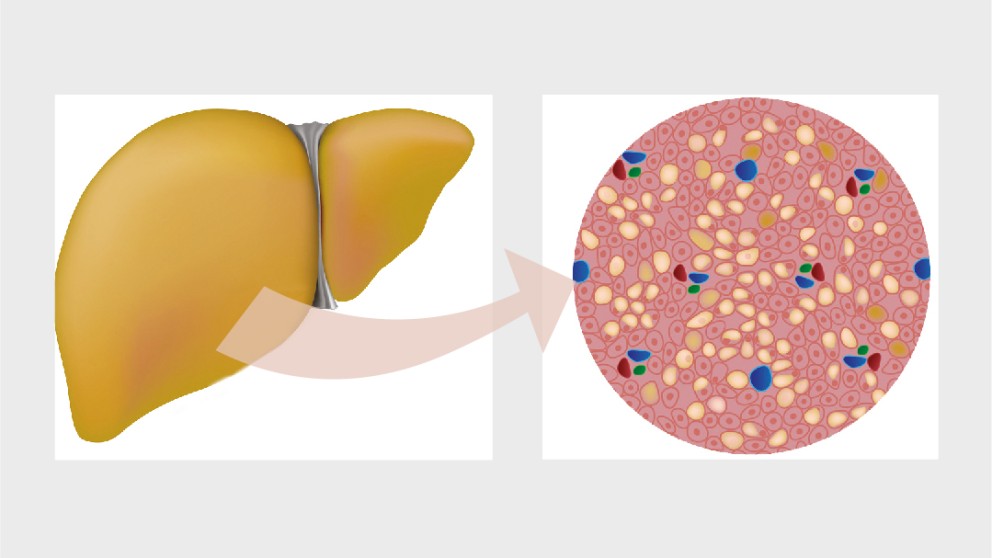
Mistakes in metabolic dysfunction associated steatotic liver disease and how to avoid them
Topics
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

Functional bowel disorders with diarrhoea: Clinical guidelines of the United European Gastroenterology and European Society for Neurogastroenterology and Motility
Publisher
Guideline
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

ESPEN guideline on clinical nutrition and hydration in geriatrics
Dorothee Volkert, Anne Marie Beck, Tommy Cederholm, Alfonso Cruz-Jentoft, Sabine Goisser, Lee Hooper, Eva Kiesswetter, Marcello Maggio, Agathe Raynaud-Simon, C. Sieber, Lubos Sobotka, Dieneke van Asselt, Rainer Wirth, Stephan Bischoff
Publisher
Guideline
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

Nutrition in Pediatric Inflammatory Bowel Disease: A Position Paper on Behalf of the Porto Inflammatory Bowel Disease Group of the European Society of Pediatric Gastroenterology, Hepatology and Nutrition
Erasmo Miele, Raanan Shamir, Marina Aloi, Amit Assa, Christian Braegger, Jiri Bronsky, Lissy de Ridder, Johanna Escher, Iva Hojsak, Sanja Kolacek, Sibylle Koletzko, Arie Levine, Paolo Lionetti, Massimo Martinelli, Frank Ruemmele, Richard K Russell, Rotem Boneh, Johan E. van Limbergen, Gigi Veereman, Annamaria Staiano