Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
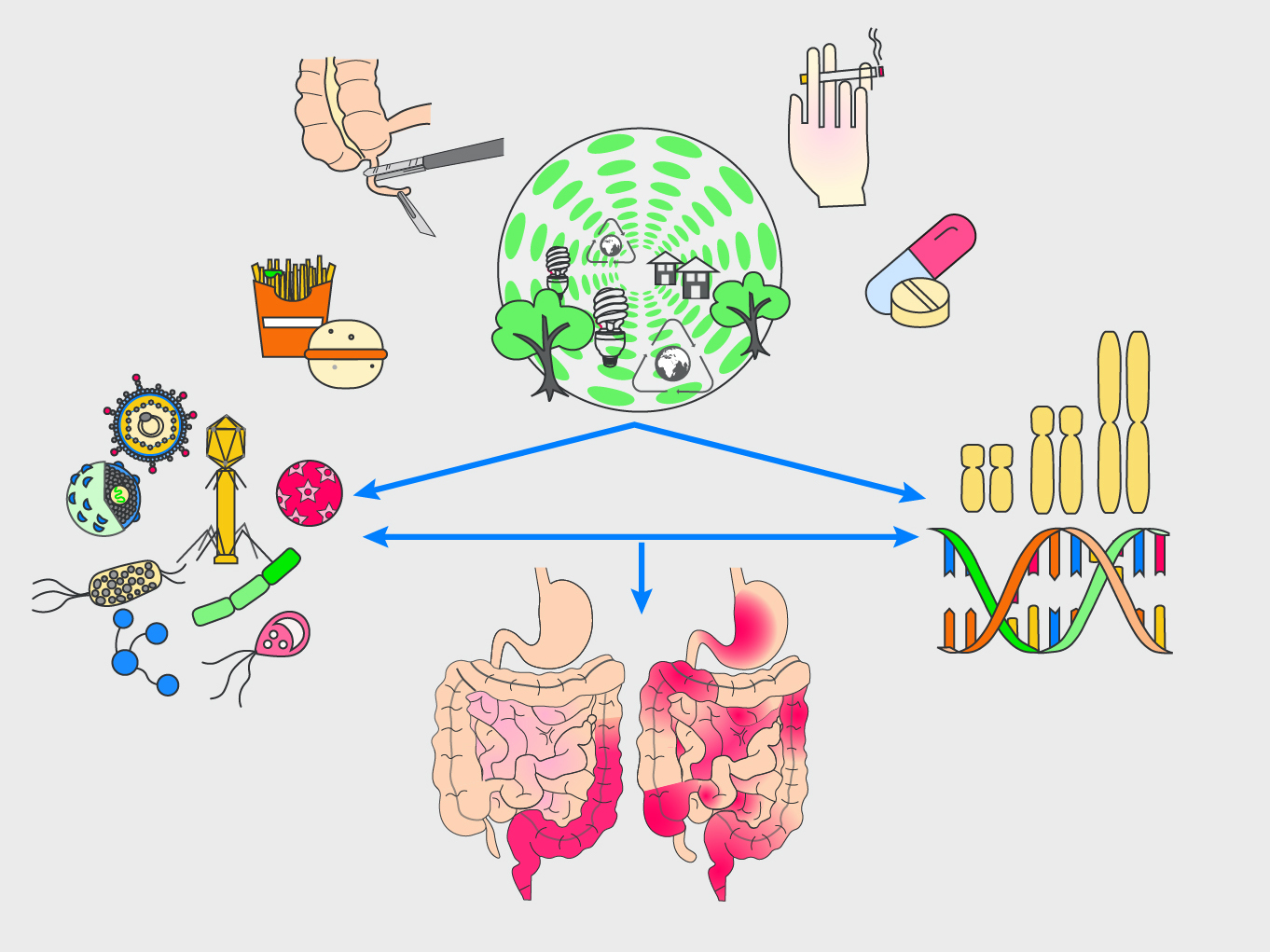
IBD epidemiology & aetiology
Event
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

Acute pancreatitis
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
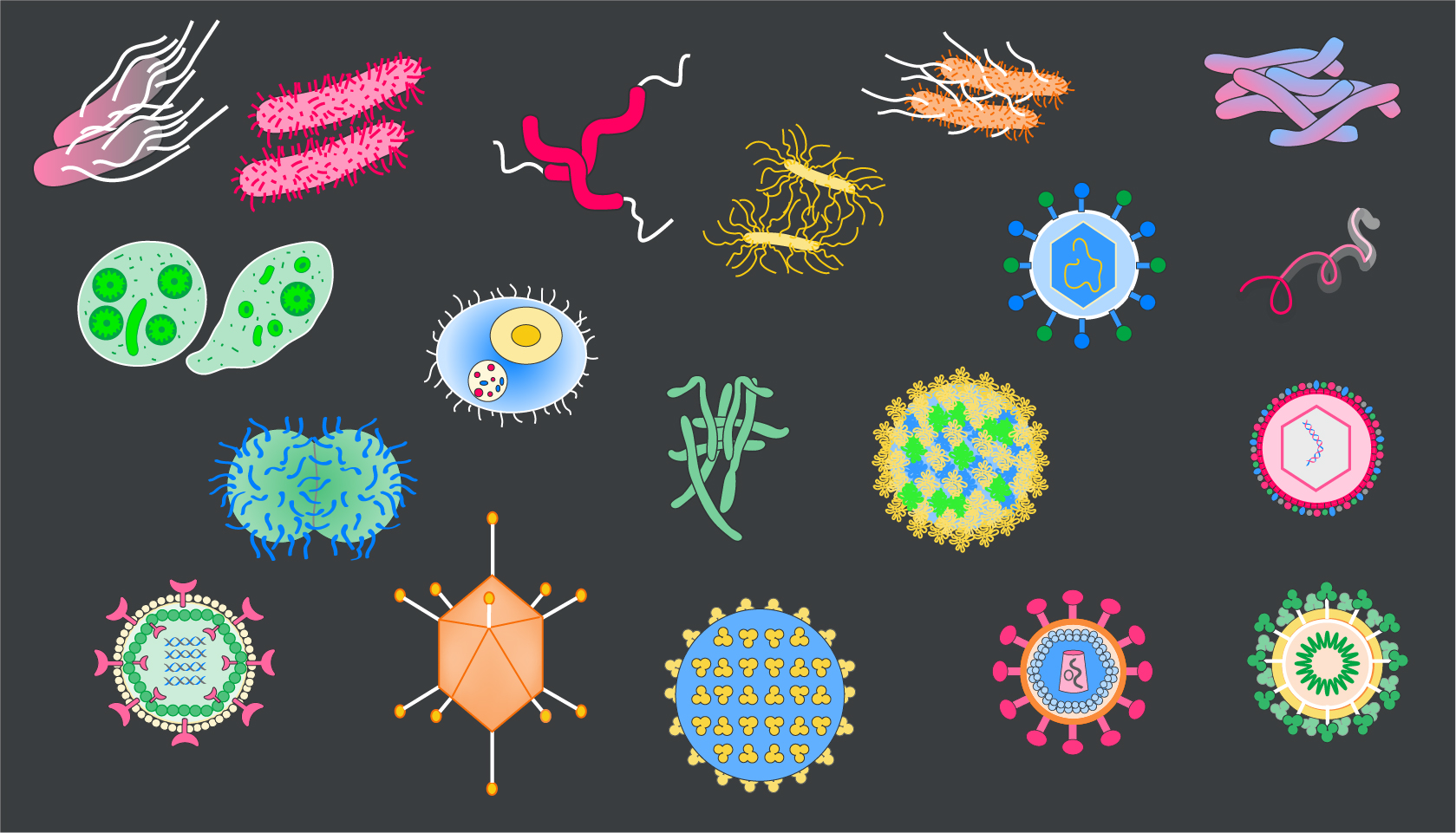
Infectious Colitis
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

CHARACTERISTICS OF LEISHMANIA INFECTION IN PATIENTS WITH INFLAMMATORY BOWEL DISEASE
Lucía Madero 1, JOSE MANUEL BENITEZ CANTERO 2, ALEJANDRO MÍNGUEZ SABATER 3, Luis Fernando Mayorga Ayala 4, José Joaquín Ramirez Palanca 5, Nadia Moreno Sanchéz 6, Cirilo Amorós García. 7, M. Ángeles Nieto Vitoria 8, Raquel Mena 9, Leticia Gimeno Pitarch 10, Nuria Maroto Arce 11, Carles Suria Bolufer 12, Francisco Rodriguez-Moranta. 13, Ingrid Ordás 14, Lucía Ruiz Sánchez 15, Miguel García-Brenes 16, Albert Martin-Cardona 17, Cristina Rubín de Célix 18, Daniel Ginard 19, Karina Cárdenas-Jaén 20, Lucia Medina-Prado 21, Noemi Pedrero Leparmentier 22, Maria del Rocio Plaza Santos 23, Rosario Salmoral Luque 24, Teresa de Jesús Martínez-Pérez 25, Virginia Algara Soriano 26, Yamile Zabana 27, Ana Gutiérrez Casbas 28
1 Hospital General Universitario Doctor Balmis, Alicante. ISABIAL., Alicante, Spain
2 Hospital Universitario Reina Sofía, IMIBIC (Córdoba), Córdoba, Spain
3 Hospital Universitari i Politécnic la Fe, Valencia, Spain
4 Unitat d’Atenció Crohn-Colitis, Servei d'Aparell Digestiu, Hospital Universitari Vall d'Hebron, Barcelona, Spain, Barcelona, Spain
5 Hospital Lluis Alcanyis (Xativa), Algemesí, Spain
6 Hospital Doctor Peset de Valencia., Valencia, Spain
7 Hospital Arnau de Vilanova, Valencia, Valencia, Spain
8 Hospital Reina Sofía, Murcia., Murcia, Spain
9 Consorci Sanitari de Terrassa, Terrassa, Spain
10 Hospital General Universitario de Castellón, Castellón, Spain
11 H. de lhorta-manises, Manises, Spain
12 Hospital Clínico Universitario de Valencia., Valencia, Spain
13 Unidad de EII del Servicio de Gastroenterologia, Hospital Universitario Bellvitge, IDIBELL, Hospitalet de Llobregat, Barcelona, Spain
14 Hospital Clinic of Barcelona, Barcelona, Spain
15 Hospital General Universitario de Valencia. Gastroenterología., Valencia, Spain
16 Inflammatory Bowel Disease Unit, Gastroenterology Department, Hospital Clínico San Carlos and Instituto de Investigación del Hospital Clínico San Carlos [IdISSC], Madrid, Spain., Madrid, Spain
17 Hospital Universitari Mútua Terrassa, Centro de Investigación biomédica en red de enfermedades hepáticas y digestivas (CIBERehd), Terrasa (Barcelona), Spain
18 Hospital Universitario de La Princesa, Madrid, Spain
19 Hospital Universitario Son Espases, Palma de Mallorca, Spain
20 Hospital Virgen de Los Lirios., Alcoy, Spain
21 Hospital Marina Baixa, Villajoyosa, Alicante, Spain
22 Hospital General Universitario Santa Lucía, Cartagena, Murcia, Cartagena, Murcia, Spain
23 H. Infanta Leonor, Madrid, Spain
24 Hospital General Universitario de Toledo, Toledo, Spain
25 Hospital Virgen de Luz, Cuenca, Spain
26 Hospital Vinalopó, Elche, Alicante, Spain
27 Hospital Universitari Mútua Terrassa. entro de Investigación Biomédica en Red en Enfermedades Hepáticas y Digestivas (CIBERehd), Terrassa, Spain
28 Hospital General Universitario Doctor Balmis, Alicante. ISABIAL. CIBERehd, Alicante, Spain
Conference
Topics
Submission format
Session
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
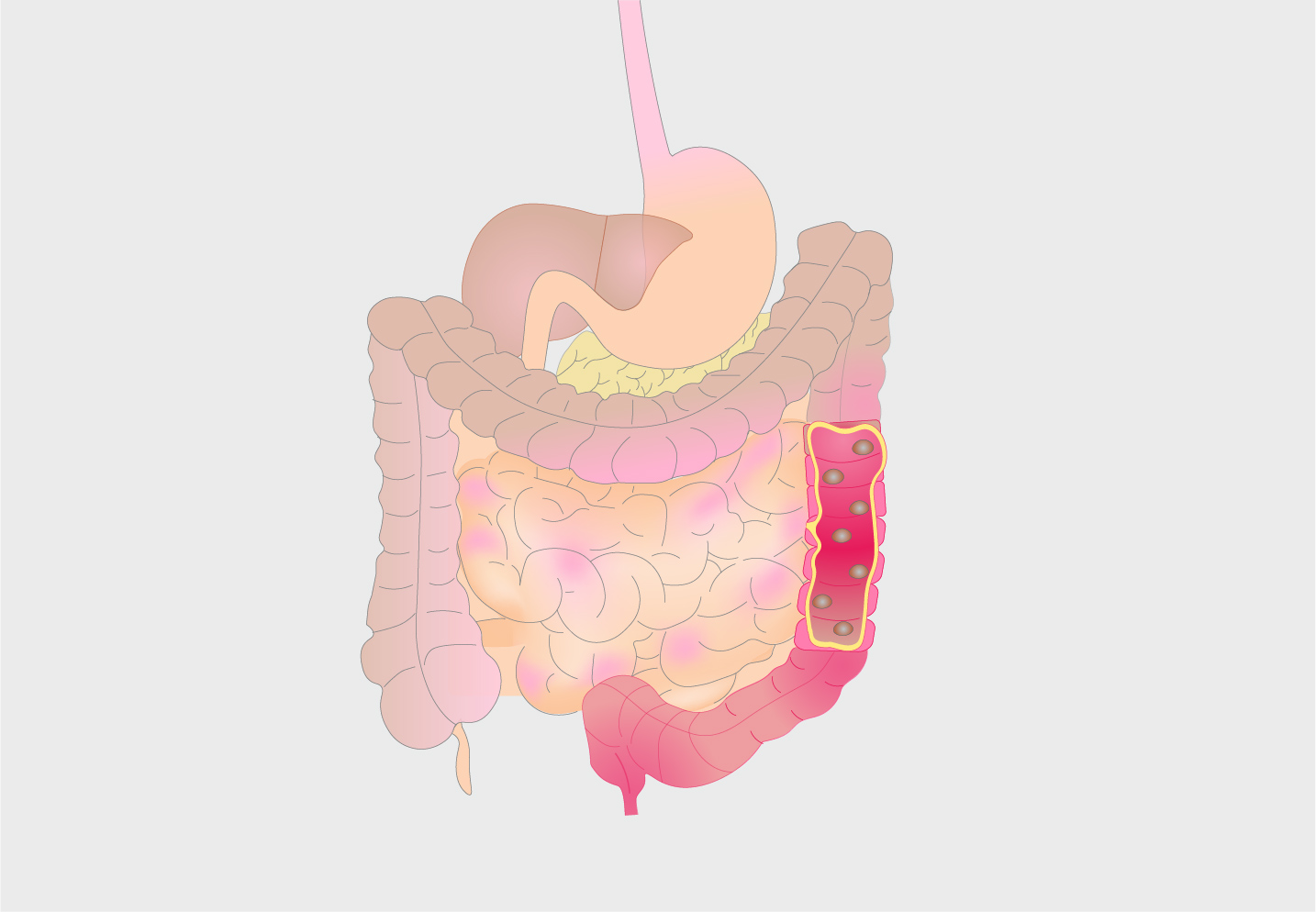
Ulcerative Colitis
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

DFL23806, A SELECTIVE AGONIST OF GPR120, DISPLAYS UNIQUE PHARMACOLOGICAL POTENTIAL AND INHIBITS ACUTE AND CHRONIC COLITIS IN MURINE MODELS
RAFAEL CYPRIANO DUTRA 1, Gianluca Bianchini 1, Rubina Novelli 1, Pier Giorgio Amendola 1, Sarah Carty 1, Giada Cremonesi 1, Andrea Aramini 1
1 Dompé Farmaceutici S.p.A., Napoli, Italy
Conference
Topics
Submission format
Session
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

ANTI-INFLAMMATORY EFFECT OF LMT503, A MODULATOR OF CELL METABOLISM, AMELIORATES MURINE ADOPTIVE T CELL TRANSFER-INDUCED COLITIS
1 Graduate School of Medical Science, Brain Korea 21 Project, Yonsei University College of Medicine, Seoul, Korea, Republic of
2 Graduate School of Medical Science, Brain Korea 21 Project, Yonsei University College of Medicine, Seoul, Korea, Republic of|||Severance Biomedical Science Institute, Yonsei University College of Medicine, Seoul, Korea, Republic of
Conference
Topics
Submission format
Session