Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

Gastric polyps
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
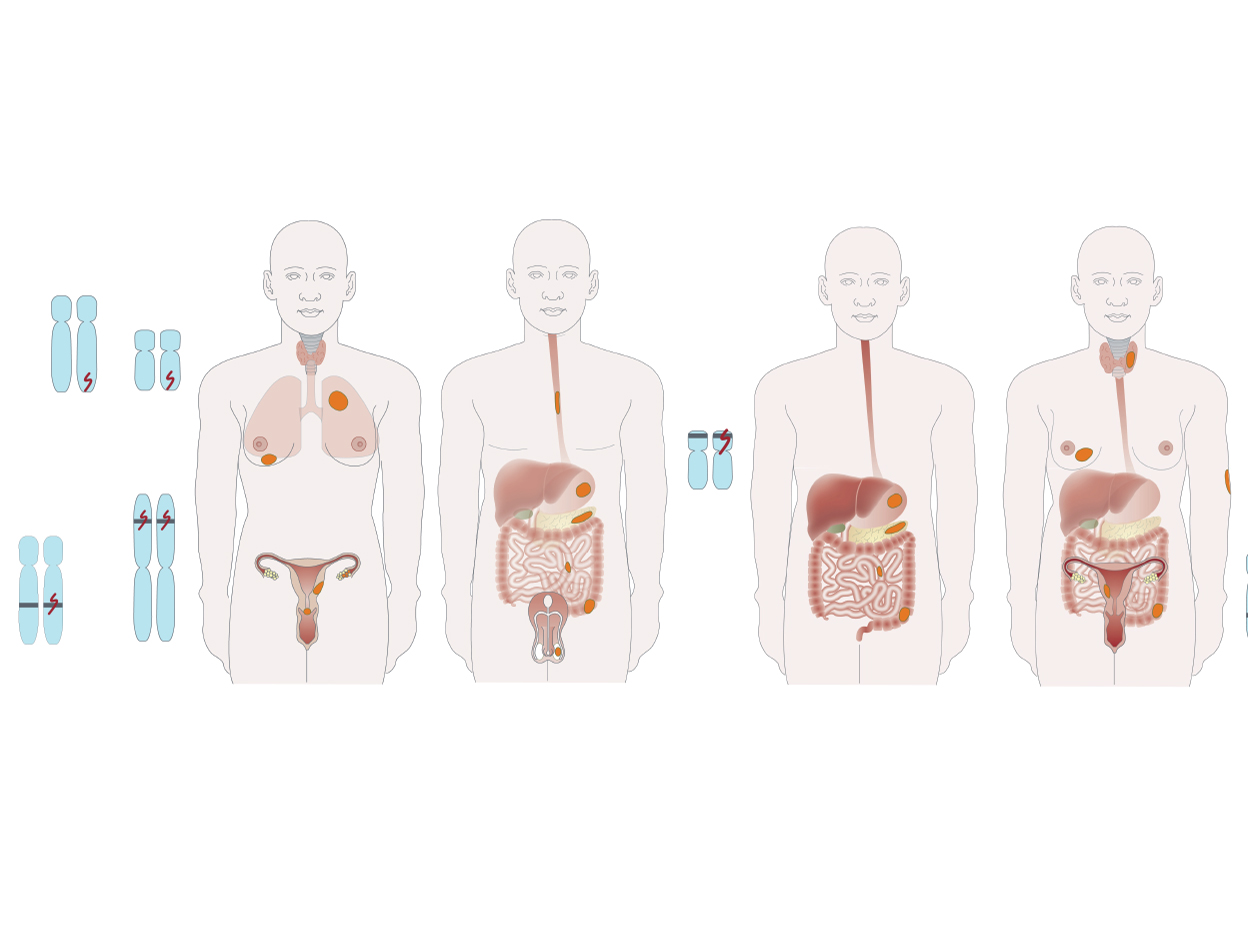
Hereditary gastrointestinal polyposis syndromes
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
Best of UEG Week - Nursing with Mary Phillips and Leigh Donnelly
Topics
Published

Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
Oligometastatic disease: Can the surgeon prolong life expectancy
1 Università Vita-Salute San Raffaele, San Raffaele, Italy
Event
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

AUTOMATICALLY OPTIMIZED RADIOMICS MODELING SYSTEM FOR SMALL GASTRIC SUBMUCOSAL TUMORS (<2CM) DISCRIMINATION BASED ON ENDOSCOPIC ULTRASOUND IMAGES
Mingyan Cai 1, Baohui Song 1, Pingting Gao 1, Yunshi Zhong 1, Yinhui Deng 2, Jinhua Yu 2, Pinghong Zhou 1
1 Zhongshan Hospital, Fudan Univeristy, Shanghai, China
2 Fudan University, Shanghai, China
Conference
Topics
Submission format
Session
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

THE EFFECTS OF SODIUM BUTYRATE SUPPLEMENTATION ON THE SEVERITY OF ABDOMINAL SYMPTOMS AND CARBOHYDRATE METABOLISM IN PATIENTS WITH TYPE 2 DIABETES - PRELIMINARY DATA
Paulina Panufnik 1, Martyna Więcek 1, Paulina Szwarc 1, Magdalena Kaniewska 1, Konrad Lewandowski 1, Edward Franek 2, Grazyna Rydzewska Wyszkowska 3
1 National Medical Institute of the Ministry of the Interior and Administration in Warsaw, Warsaw, Poland
2 National Medical Institute of the Ministry of the Interior and Administration in Warsaw, Warsaw, Poland|||Department of Human Epigenetics, Mossakowski Medical Research Institute, Warsaw, Poland
3 National Medical Institute of the Ministry of the Interior and Administration in Warsaw, Warsaw, Poland|||Collegium Medicum of Jan Kochanowski University, Kielce, Poland
Conference
Topics
Submission format
Session
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
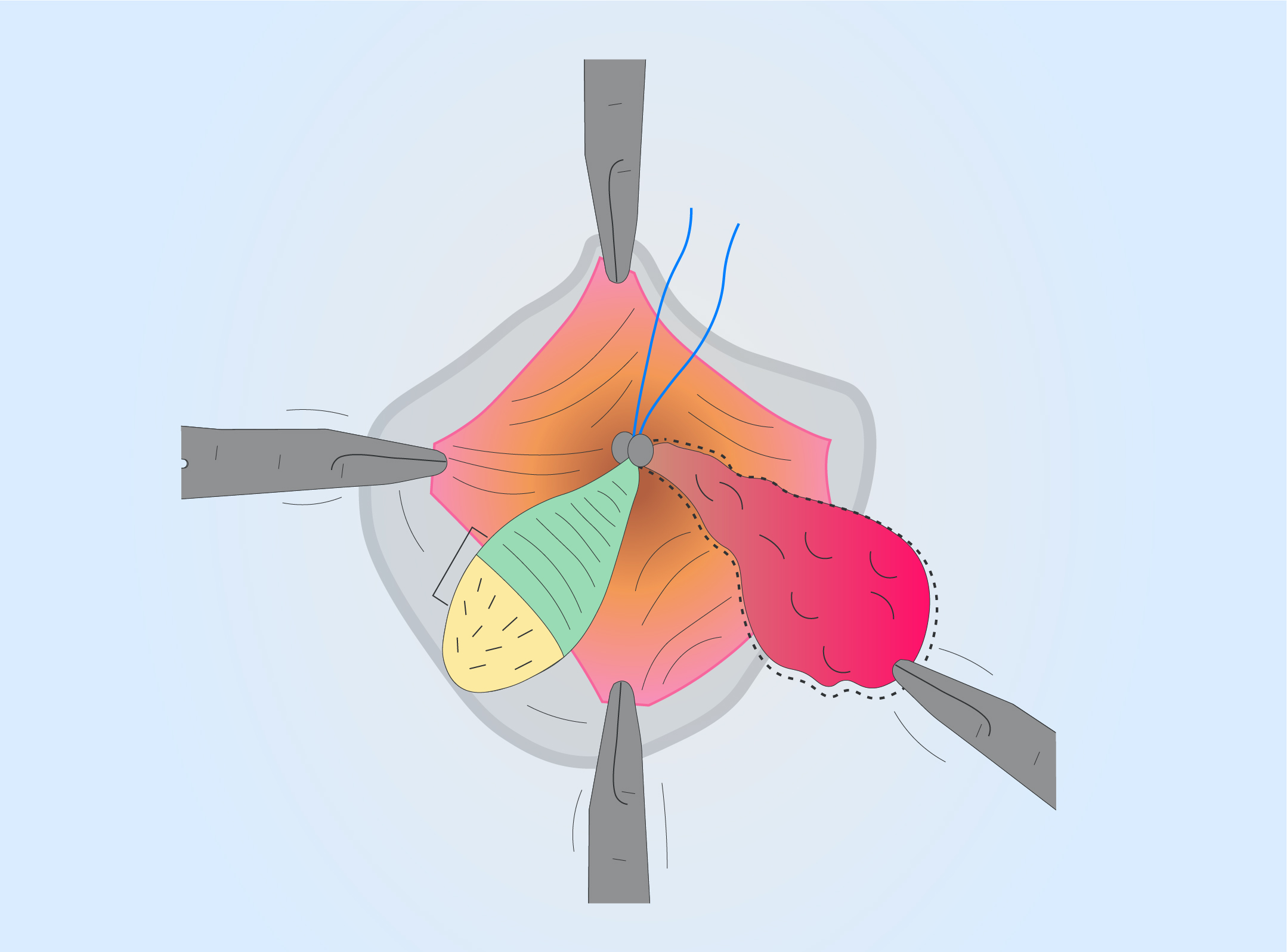
Proctology — haemorrhoids and perianal skin conditions
Event
Topics