Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.
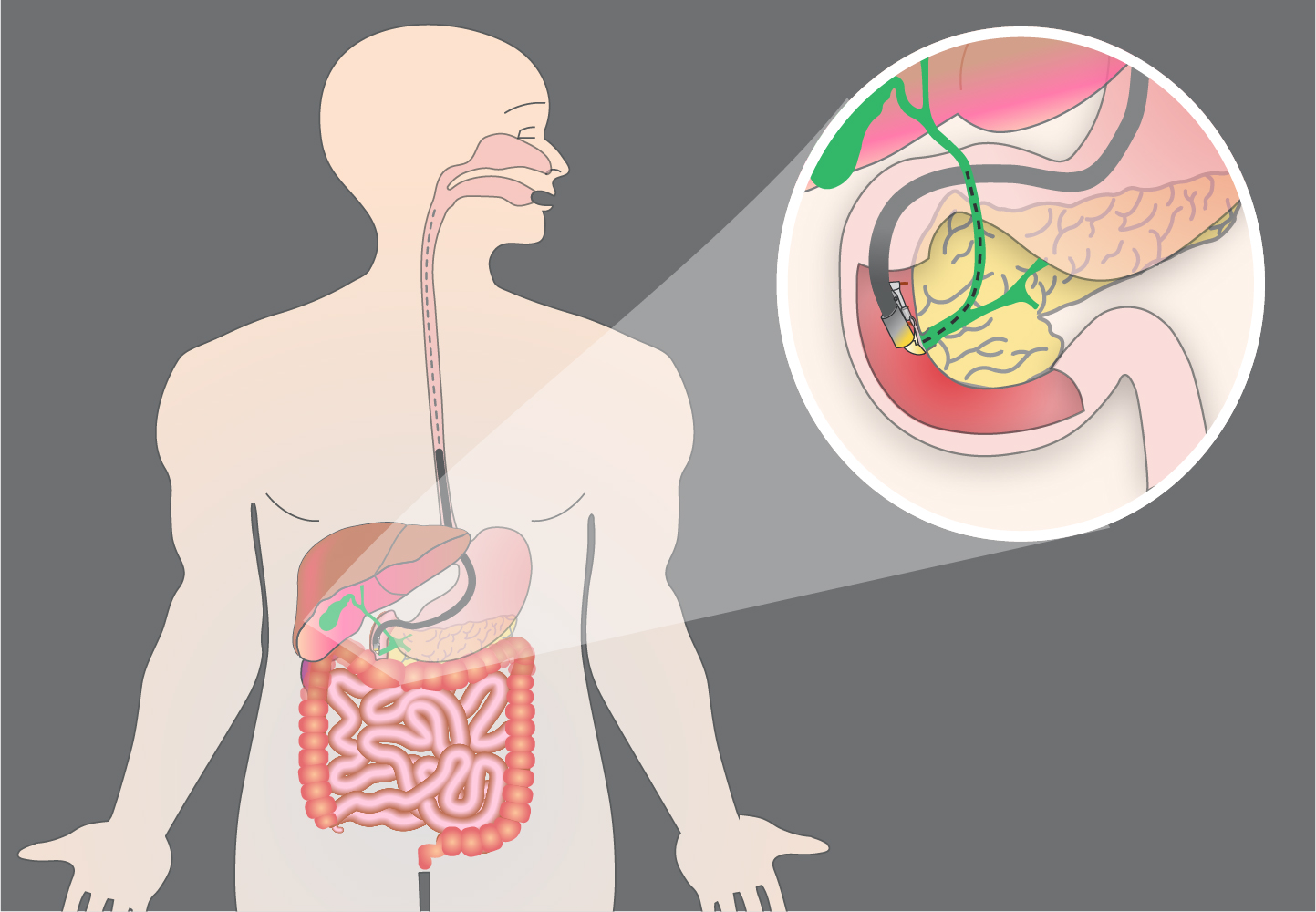
Advanced ERCP - Part 2
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

Advanced ERCP - Part 1
Event
Topics
Accreditation status
Duration
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

ASSESSING ENDOSCOPIC TRAINING IN GASTROENTEROLOGY FELLOWSHIPS: A MULTICENTRIC CROSS SECTIONAL PILOT STUDY
Amine Achemlal 1, Nejjari Fouad 1, salma ouahid 1, Salma Azammam 1, Meriem Amine 1, Sakina Oualaalou 1, chaimae jioua 1, Bangda Yannick 1, Rachid Laroussi 1, Abdelfettah Touibi 1, Tarik ADIOUI 1, Mouna Tamzaourte 1
1 Mohamed V Military Training Hospital, Rabat, Morocco
Conference
Submission format
Session
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

FEASIBILITY AND SAFETY OF SINGLE ORAL CHOLEDOSCOPY COMBINED WITH ENDOSCOPIC RADIOFREQUENCY ABLATION FOR THE DIAGNOSIS AND TREATMENT OF UNRESECTABLE EXTRAHEPATIC BILE DUCT CARCINOMA
1 Hangzhou First People’s Hospital, Hangzhou, China|||Department of Gastroenterology, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China|||Key Laboratory of Integrated Traditional Chinese and Western Medici
Conference
Topics
Submission format
Session
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

ENDOSCOPIC SUBMUCOSAL DISSECTION OF APPENDICULAR LESIONS IS FEASIBLE AND SAFE: A RETROSPECTIVE MULTICENTER STUDY
Mariana Figueiredo Ferreira 1, Clara Yzet 2, Thimothée Wallenhorst 3, Jerome Rivory 4, Florian Rostain 4, Marion SCHAEFER 5, Jean-Baptiste Chevaux 6, Sarah Leblanc 7, Vincent Lepilliez 7, Félix Corre 8, Gabriel Rahmi 9, Jérémie Jacques 10, Jeremie Albouys 11, Mathieu Pioche 4
1 Saint-Pierre University Hospital, Brussels, Belgium
2 Amiens University Hospital, Amiens, France
3 CHU Rennes, Rennes, France
4 Hospices civils de Lyon, Lyon, France
5 Centre Hospitalier Régional Universitaire de Nancy, Nancy, France
6 University Hospital of Nancy, Vandoeuvre Les Nancy, France
7 Hôpital Privé Jean Mermoz, Sainte Foy Les Lyon, France
8 Cochin Hospital, Paris, France
9 Hôpital Européen Georges Pompidou Dept. de Gastroenterologie, Paris, France
10 CHU Limoges - Hepato-Gastro-Enterology, CHU Limoges, Limoges, France
11 CHU Limoges / University of Limoges, Limoges, France
Conference
Topics
Submission format
Citation
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

LEARNING FROM A CASE OF PAINLESS OBSTRUCTIVE JAUNDICE
1 University Hospitals Nottingham and University of Nottingham, Nottingham, United Kingdom
Conference
Topics
Submission format
Session
Published
Log in to access this content.
Free for all myUEG account holders. Your access level is set automatically based on your occupation. Medical professionals get full access to all content. If you are a non-medical user, you can only access UEG Week content from congresses you attended.
Not sure what you can access? Learn more about account types.

THE LONG-TERM EFFECT ON SURGERY-FREE SURVIVAL OF BIOLOGICAL COMPARED TO CONVENTIONAL THERAPY IN CROHN’S DISEASE IN REAL WORLD-DATA: A PROPENSITY-SCORE MATCHED STUDY
Marco Valvano 1, Antonio Vinci 2, Marta Ameli 1, Nicola Cesaro 1, sara FRASSINO 1, Angelo Viscido 1, Stefano Necozione 1, Giovanni Latella 1
1 Università degli Studi di L'Aquila, L'Aquila, Italy
2 University of Tor Vergata, Roma, Italy
Conference
Topics
Submission format
Session